Table of Contents
A common assumption about fasting is this:
“If I don’t eat, my blood sugar should keep falling.”
But in real physiology, blood sugar rarely collapses, even during extended fasting.
The reason is glucagon — a hormone designed to prevent dangerous hypoglycemia when food is unavailable.
Glucagon Is the Body’s Anti-Crash Hormone
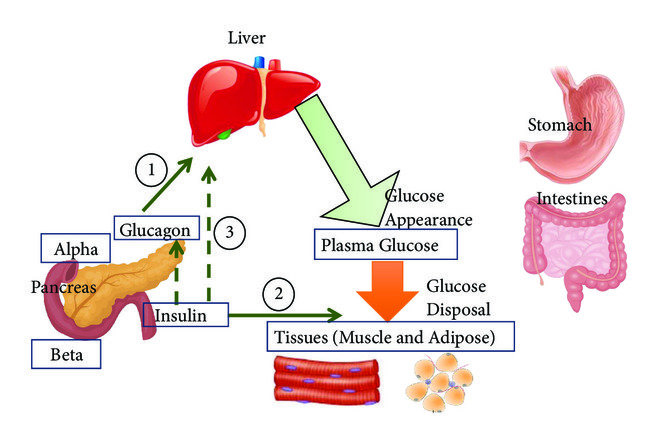
Glucagon is released by the pancreas and works as the functional opposite of insulin.
- Insulin stores energy after meals
- Glucagon releases energy during fasting
When insulin falls, glucagon rises automatically.
This switch is intentional and protective.
What Actually Triggers Glucagon During Fasting
Glucagon release is not random. It responds to clear signals:
- low insulin
- falling liver glycogen
- lack of incoming dietary glucose
- continuous glucose demand from the brain
The pancreas increases glucagon to maintain circulation glucose, not to “raise sugar unnecessarily.”
How Glucagon Prevents Blood Sugar From Dropping to Zero
Glucagon acts mainly on the liver.
It instructs the liver to:
- release stored glucose from glycogen
- keep blood glucose within a survivable range
- later, produce glucose when stores run low
This explains why fasting blood sugar stays stable instead of collapsing.
Glycogen First, Then Glucose Production
Early fasting:
- glucagon mobilizes glycogen
Later fasting:
- glycogen becomes depleted
- glucagon shifts metabolism to gluconeogenesis
Glucose is made from:
- glycerol from fat
- lactate
- selected amino acids
This process is regulated, not excessive.
Why Blood Sugar Can Look “Normal” or Slightly High
Some people notice:
- normal fasting glucose
- or slightly elevated morning glucose
- despite extended fasting
This does not mean fasting is failing.
Glucagon’s goal is adequate glucose, especially for:
- the brain
- red blood cells
- nervous tissue
It does not aim for the lowest possible reading.
How Glucagon Interacts With Other Fasting Hormones
During fasting, glucagon works alongside:
- growth hormone (muscle preservation)
- cortisol (stress adaptation)
- adrenaline (energy availability)
Together, these hormones prioritize survival, not numerical glucose targets.
When Glucagon Becomes Excessive
Glucagon can become problematic when:
- insulin resistance is present
- stress hormones remain chronically elevated
- metabolic signaling is impaired
In these cases, glucagon may stay active longer than necessary, keeping blood sugar elevated.
This reflects metabolic context, not a flaw in fasting itself.
The Core Insight
Blood sugar does not drop to zero during fasting because the body is designed to prevent that outcome.
Glucagon:
- stabilizes glucose
- protects the brain
- enables safe fasting
Low insulin allows fasting.
Glucagon makes fasting survivable.
Final Summary
During fasting:
- insulin decreases
- glucagon increases
- the liver supplies glucose
This balance keeps blood sugar stable, not zero.
That is normal physiology.
