Table of Contents
Introduction
Fasting does not only affect insulin. It also influences stress hormones, particularly cortisol, which plays a major role in blood sugar regulation. Understanding how cortisol responds to fasting helps explain why some people see rising blood sugar levels, feel fatigued, or experience stress-related symptoms while fasting.
This article explains how fasting affects cortisol, why cortisol can raise blood sugar, and how stress hormone responses differ between individuals.
What Cortisol Does in the Body
Cortisol is a hormone released by the adrenal glands in response to physical or psychological stress. Its primary role is to ensure adequate energy availability by increasing glucose production in the liver.
Under normal conditions, cortisol follows a daily rhythm—higher in the morning and lower at night. This rhythm supports wakefulness, energy balance, and metabolic stability.
How Fasting Influences Cortisol Levels
Fasting can act as a physiological stressor, especially when combined with calorie restriction, intense exercise, or poor sleep. In response, the body may increase cortisol release to maintain blood glucose levels.
For some individuals, fasting leads to stable cortisol patterns. For others, cortisol rises during fasting, particularly when the body perceives an energy shortage.
This explains why fasting outcomes vary even when insulin levels are low.
Why Cortisol Can Raise Blood Sugar During Fasting
Cortisol increases blood sugar by:
- Stimulating gluconeogenesis in the liver
- Reducing glucose uptake in peripheral tissues
- Supporting stress-driven energy release
When cortisol remains elevated, blood sugar can rise despite the absence of food intake. This response is protective in the short term but can become problematic if sustained.
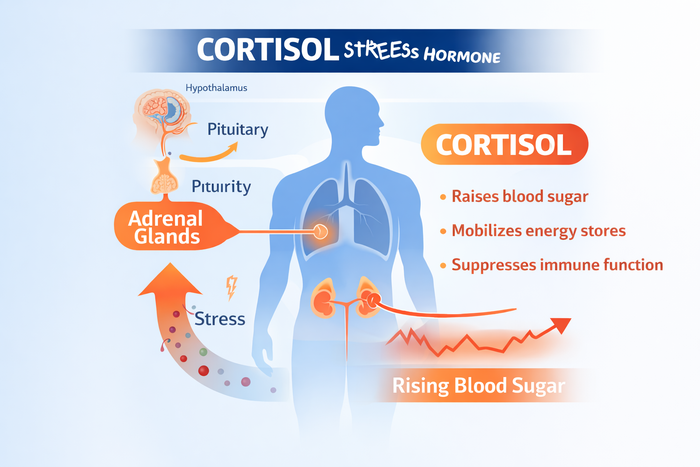
Cortisol, Insulin, and Metabolic Response
Cortisol and insulin interact closely. Elevated cortisol can reduce insulin sensitivity, making it harder for cells to absorb glucose efficiently. This interaction explains why fasting does not always improve blood sugar control, even when insulin levels are reduced.
The combined effect of low insulin and high cortisol can produce unexpected blood sugar readings during fasting.
Cortisol and Fasting: Why Stress Hormones Can Raise Blood Sugar
Fasting has become one of the most popular health strategies for improving metabolic health, losing weight, and stabilizing blood sugar. From intermittent fasting to extended fasts, many people expect lower glucose levels as a natural result of not eating. Yet for a surprising number of individuals, fasting does the opposite—it raises blood sugar.
The culprit is often cortisol, the body’s primary stress hormone.
Understanding how cortisol interacts with fasting is essential if you want to use fasting effectively without sabotaging your metabolic goals. In this article, we’ll explore the science behind cortisol, why fasting can increase stress hormones, and how that stress response can raise blood sugar—even when you haven’t eaten a single calorie.
What Is Cortisol?
Cortisol is a steroid hormone produced by the adrenal glands, which sit on top of your kidneys. It plays a critical role in survival by helping the body respond to stress—both physical and psychological.
Cortisol affects nearly every system in the body, including:
- Blood sugar regulation
- Inflammation and immune response
- Blood pressure
- Energy metabolism
- Sleep–wake cycles
Under normal conditions, cortisol follows a diurnal rhythm. Levels are highest in the early morning (helping you wake up) and gradually decline throughout the day, reaching their lowest point at night.
This rhythm is tightly regulated by the hypothalamic-pituitary-adrenal (HPA) axis, a complex feedback system that responds to stress and energy availability.
Why Cortisol Exists: A Survival Hormone
From an evolutionary perspective, cortisol is not “bad.” It exists to keep you alive.
When the brain senses danger—whether it’s a predator, infection, injury, or lack of food—it signals the adrenal glands to release cortisol. One of cortisol’s main jobs is to increase available energy, especially glucose.
It does this by:
- Stimulating gluconeogenesis (the production of glucose from amino acids in the liver)
- Reducing insulin sensitivity
- Mobilizing stored energy (fat and muscle tissue)
This response made sense when humans faced starvation or physical threats. However, in modern life, chronic stress and aggressive fasting can trigger cortisol repeatedly—sometimes unnecessarily.
How Fasting Affects Cortisol Levels
Fasting is a form of controlled stress. When done appropriately, it can improve insulin sensitivity, enhance fat burning, and promote metabolic flexibility. But fasting also sends a signal to the brain that food is unavailable.
For some people, especially those already under high stress, this signal can increase cortisol production.
Short-Term vs Long-Term Fasting Stress
- Short-term fasting (12–16 hours)
Often well tolerated and may not significantly raise cortisol in healthy individuals. - Extended fasting (18+ hours or multi-day fasts)
Can increase cortisol, especially if combined with calorie restriction, intense exercise, or poor sleep. - Calorie deficit + fasting
A common mistake that amplifies stress hormone release.
When cortisol rises during fasting, blood sugar may increase instead of decrease.
Why Cortisol Raises Blood Sugar During Fasting
Many people are confused when they see elevated glucose readings while fasting. After all, if no food is entering the body, where is the sugar coming from?
The answer lies in cortisol-driven glucose production.
1. Cortisol Stimulates Gluconeogenesis
Cortisol tells the liver to produce glucose from non-carbohydrate sources such as:
- Amino acids (from muscle tissue)
- Lactate
- Glycerol (from fat breakdown)
This process ensures that vital organs—especially the brain—have access to glucose during times of stress or food scarcity.
2. Cortisol Reduces Insulin Sensitivity
Cortisol makes cells temporarily more resistant to insulin. This ensures glucose stays in the bloodstream rather than being stored, keeping energy readily available.
In fasting individuals, this can show up as:
- Elevated fasting glucose
- Higher morning blood sugar
- Poor glucose response despite low carbohydrate intake
3. The Dawn Phenomenon
Cortisol naturally rises in the early morning hours. In some people, this cortisol surge causes a noticeable increase in blood sugar upon waking—a phenomenon known as the dawn effect.
Fasting can exaggerate this effect, especially in individuals with insulin resistance or high baseline stress.
Who Is Most Affected by Cortisol Spikes During Fasting?
Not everyone experiences cortisol-driven blood sugar increases during fasting. Certain populations are more vulnerable.
1. People With Chronic Stress
Work stress, emotional stress, poor sleep, and overtraining all elevate baseline cortisol levels. Adding fasting on top of this can push cortisol even higher.
2. Individuals With Insulin Resistance or Prediabetes
When insulin sensitivity is already impaired, cortisol’s glucose-raising effects become more pronounced.
3. Women (Especially Under-Eating)
Women are generally more sensitive to energy deficits. Aggressive fasting combined with low calorie intake can disrupt hormones and raise cortisol more easily.
4. Over-Exercisers
High-intensity training plus fasting is a potent cortisol trigger. Without adequate recovery and nutrition, blood sugar dysregulation is common.
Signs Cortisol May Be Sabotaging Your Fasting Results
You may be dealing with cortisol-related blood sugar issues if you notice:
- Higher fasting glucose than expected
- Elevated morning blood sugar despite low-carb eating
- Feeling wired but tired
- Sleep disturbances
- Anxiety or irritability while fasting
- Stalled fat loss despite calorie control
These are signs your body perceives fasting as a threat rather than a beneficial stimulus.
Is Cortisol Always Bad During Fasting?
No. A moderate cortisol response is normal and even beneficial. Problems arise when cortisol remains chronically elevated.
Healthy fasting should:
- Improve insulin sensitivity over time
- Reduce average blood glucose
- Enhance metabolic flexibility
If fasting is consistently raising your blood sugar, it’s a sign your approach may need adjustment—not that fasting itself is harmful.
How to Lower Cortisol While Fasting
1. Shorten Your Fasting Window
If you’re doing 18–20 hour fasts, consider reducing to 12–14 hours. This often lowers cortisol without eliminating fasting benefits.
2. Avoid Excessive Calorie Restriction
Fasting is about timing, not starvation. Eating too little during your feeding window increases stress hormone output.
3. Prioritize Sleep
Poor sleep raises cortisol dramatically. Even the best fasting protocol will fail if sleep is inadequate.
4. Reduce High-Intensity Exercise While Fasting
Replace fasted HIIT sessions with:
- Walking
- Light resistance training
- Mobility work
Save intense workouts for fed states.
5. Increase Protein Intake
Adequate protein helps blunt cortisol and prevents excessive muscle breakdown during fasting.
6. Practice Stress Reduction
Breathing exercises, meditation, and sunlight exposure all help regulate the HPA axis and cortisol output.
Cortisol, Fasting, and Long-Term Metabolic Health
The goal of fasting is metabolic resilience—not constant stress. When fasting is aligned with your lifestyle, stress levels, and nutritional needs, cortisol remains balanced and blood sugar improves.
According to research summarized by organizations like National Institutes of Health and Harvard Medical School, chronic stress plays a significant role in insulin resistance and glucose dysregulation.
This means managing cortisol is just as important as managing carbohydrates.
Key Takeaway
Fasting can influence cortisol differently depending on stress load, metabolic health, and individual hormone balance. When cortisol rises during fasting, blood sugar may increase as a protective response. Understanding this stress-hormone pathway helps explain why fasting feels beneficial for some people and challenging for others.
