Table of Contents
Introduction
Fasting is often discussed as a way to control blood sugar, lose fat, or improve metabolic health. However, the real driver behind these effects is not fasting itself—it’s how fasting changes insulin behavior in the body. Understanding how insulin responds during fasting helps explain why blood sugar improves for some people, stays high for others, and reacts differently depending on metabolic health.
This article explains how fasting affects insulin levels, what peripheral insulin resistance means, and why blood sugar responses during fasting are not the same for everyone.
What Insulin Does in the Body
Insulin is a hormone that allows glucose to move from the bloodstream into cells, where it is used for energy or stored. When insulin works efficiently, blood sugar levels remain stable. When insulin signaling is impaired, glucose stays in the blood, leading to higher readings even when food intake is low.
Insulin does not act in isolation. Its effectiveness depends on how responsive tissues like muscle and liver are to insulin signals.
How Fasting Changes Insulin Levels
During fasting, insulin levels naturally decline because no carbohydrates are being consumed. This drop in insulin is often seen as beneficial, but lower insulin does not automatically mean better insulin sensitivity.
Fasting reduces insulin secretion, but how tissues respond to insulin during this time is what determines blood sugar outcomes. In metabolically healthy individuals, fasting improves insulin efficiency. In others, insulin resistance may persist despite low insulin levels.
Peripheral Insulin Resistance Explained
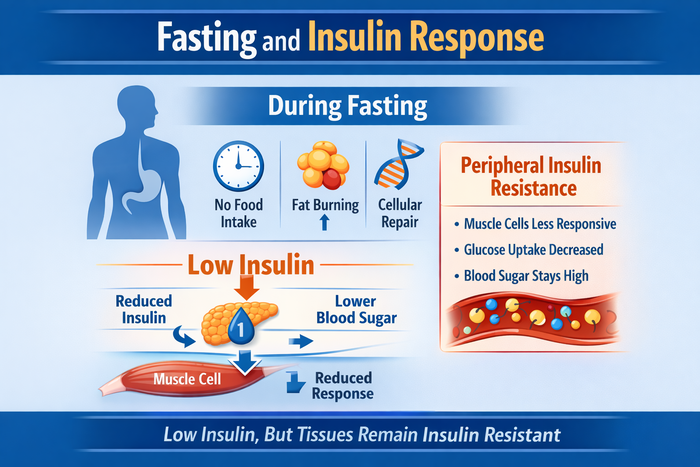
Peripheral insulin resistance refers to reduced insulin responsiveness in tissues such as skeletal muscle. Even when insulin levels are low during fasting, glucose uptake by muscles may remain impaired. This can cause blood sugar to stay elevated despite fasting.
As explained in the referenced video by Thomas DeLauer, insulin resistance can be tissue-specific. This explains why fasting improves blood sugar in some people while others see little change.
Why Blood Sugar Can Stay High During Fasting
Several mechanisms can keep blood sugar elevated during fasting:
- The liver releases stored glucose through gluconeogenesis
- Muscle tissue remains insulin resistant
- Stress hormones like cortisol increase glucose output
These processes are normal survival mechanisms but become problematic when insulin signaling is already impaired.
This explains why fasting alone does not always resolve blood sugar issues.
How This Connects Fasting, Hormones, and Metabolism
Fasting influences multiple hormones at once. While insulin decreases, other hormones adjust to maintain energy balance. The overall metabolic response depends on insulin sensitivity, hormone balance, and tissue health.
Understanding insulin behavior during fasting helps set realistic expectations and explains why fasting results vary from person to person.
Key Takeaway
Fasting lowers insulin levels, but improved blood sugar control depends on how well tissues respond to insulin—not just how much insulin is present. Peripheral insulin resistance can persist during fasting, explaining why some people experience stable or even elevated blood sugar levels despite not eating.
