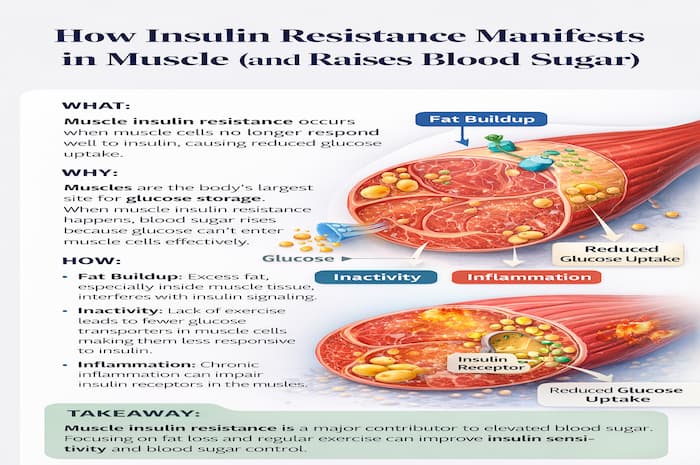
Muscle tissue plays a major role in controlling blood sugar. In fact, most of the glucose you eat is meant to be absorbed by your muscles. When muscles stop responding properly to insulin, blood sugar levels remain high — even if diet and fasting are controlled.
This article explains what muscle insulin resistance is, why it raises blood sugar, and how it develops inside muscle tissue.
What Is Muscle Insulin Resistance?
Muscle insulin resistance occurs when muscle cells no longer respond effectively to insulin. As a result, glucose cannot enter muscle cells efficiently and stays in the bloodstream.
Under normal conditions:
- Insulin signals muscle cells to absorb glucose
- Glucose is used for energy or stored as glycogen
With insulin resistance:
- The insulin signal weakens
- Muscle glucose uptake declines
- Blood sugar levels rise
Because muscle is the body’s largest glucose sink, resistance here has a strong impact on overall blood sugar control.
Why Muscle Insulin Resistance Raises Blood Sugar
Muscles are responsible for clearing a large portion of glucose after meals. When muscle insulin resistance develops:
- Glucose remains in circulation longer
- The pancreas releases more insulin to compensate
- Chronically high insulin worsens resistance
Even low-carbohydrate diets may fail to normalize blood sugar if muscle tissue cannot absorb glucose properly. This is why insulin resistance can exist even without excessive sugar intake, which explains why improving food quality is critical, not just restriction, and why foods that improve insulin sensitivity play a key role in lowering blood sugar.
How Insulin Resistance Develops in Muscle
According to metabolic explanations shared by Thomas DeLauer, muscle insulin resistance develops through several key mechanisms.
| Cause | What Happens in Muscle | Effect on Blood Sugar |
|---|---|---|
| Fat Accumulation Inside Muscle | Excess fat stored within muscle tissue interferes with insulin signaling pathways. | Glucose transport into muscle cells is reduced, leaving more sugar in the bloodstream. |
| Physical Inactivity | Reduced muscle contraction lowers glucose transporter activity in muscle cells. | Muscles become less responsive to insulin, raising blood sugar levels. |
| Chronic Inflammation | Low-grade inflammation damages insulin receptors in muscle tissue. | Insulin becomes less effective at moving glucose into muscles. |
| Impaired Glucose Transport | Disrupted insulin signaling prevents glucose transporters from reaching the cell surface. | Glucose uptake is limited, causing elevated blood sugar. |
What This Means for Blood Sugar Control
When muscle insulin resistance is present:
- Blood sugar stays elevated after meals
- Insulin levels remain high
- Fat storage increases
- Metabolic flexibility declines
Improving muscle insulin sensitivity is therefore critical for stabilizing blood sugar, especially to avoid blood sugar spikes after meals.
Key Takeaway
Muscle insulin resistance is a major driver of high blood sugar. Because muscle tissue absorbs most circulating glucose, reduced insulin responsiveness here leads to persistent glucose elevation.
Supporting muscle health through movement, fat reduction, and inflammation control plays a key role in restoring insulin sensitivity and improving blood sugar regulation.
