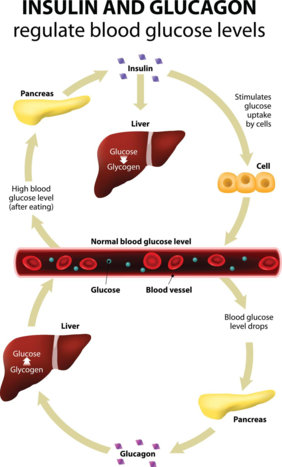
Your body is constantly switching between two metabolic states: feeding and fasting. These shifts are controlled primarily by two hormones — insulin and glucagon. Together, they regulate whether your body stores energy or releases it.
Understanding this balance explains why blood sugar rises after meals, why it stays stable during fasting, and why metabolic problems develop when the system becomes imbalanced.
For a deeper look at insulin specifically, see How Fasting Affects Insulin Levels (And Why Blood Sugar Responds Differently).
The Two Metabolic “Worlds”
After you eat, blood glucose levels rise. In response, the pancreas releases insulin.
Insulin signals your cells to:
- Absorb glucose from the bloodstream
- Store excess glucose as glycogen in the liver and muscles
- Convert extra energy into fat for storage
This is the feeding state, sometimes called the “insulin world.”
The body prioritizes storage, repair, and growth.
Several hours later, when you stop eating, blood sugar begins to fall. Now the pancreas releases glucagon — insulin’s opposite hormone.
Glucagon signals the liver to:
- Break down stored glycogen
- Release glucose back into the bloodstream
- Produce new glucose through gluconeogenesis
This is the fasting state, or the “glucagon world.”
The body shifts from storage mode to energy release mode.
Why This Balance Is Critical
Healthy metabolism depends on smooth switching between insulin and glucagon.
If insulin stays elevated for too long — due to frequent snacking, high refined carbohydrate intake, or insulin resistance — the body struggles to enter the glucagon state.
This can lead to:
- Reduced fat burning
- Increased hunger
- Weight gain
- Elevated fasting blood sugar
This mechanism helps explain why some people experience high morning glucose levels (see: Why Blood Sugar Spikes in the Morning (Dawn Phenomenon)) and why blood sugar may remain elevated during fasting (see: Why Blood Sugar Can Stay High During Fasting).
Metabolic flexibility — the ability to switch efficiently between these two hormonal states — is a key marker of metabolic health.
Does Fasting Increase Cortisol? What Actually Happens in the BodyCortisol also plays a role in maintaining blood sugar during fasting (see Does Fasting Increase Cortisol? What Actually Happens in the Body).
What Happens Step-by-Step
1️⃣ Immediately After Eating
- Blood sugar rises
- Insulin increases
- Cells absorb glucose
- Liver stores glycogen
- Fat storage increases
The body is in building and storage mode.
2️⃣ Several Hours After Eating
- Insulin levels fall
- Glucagon begins to rise
- Liver releases stored glucose
- Blood sugar remains stable
This is why healthy individuals do not experience sudden crashes between meals.
3️⃣ During Prolonged Fasting
If fasting continues:
- Glycogen stores become depleted
- Glucagon stimulates gluconeogenesis.
- Fat breakdown increases
- Ketone production rises
This phase is largely controlled by Glucagon’s Role During Fasting (Why Blood Sugar Doesn’t Drop to Zero).
At the same time, growth hormone may increase to preserve muscle mass (see: Fasting & Growth Hormone Explained (The Logical Way)).
The body becomes increasingly efficient at using stored energy.
The Bigger Picture
Insulin and glucagon are not “good” or “bad” hormones. Both are essential. Problems arise when the balance is disrupted — especially when insulin remains chronically elevated and the body rarely enters a proper fasting state.
Understanding these hormonal shifts helps clarify:
- Why intermittent fasting affects blood sugar
- Why insulin resistance develops
- Why metabolic health depends on timing, not just calories
The feeding state builds.
The fasting state releases.
Health depends on the rhythm between the two.
